Caso Clínico
Bilateral jaw fracture after long term treatment with bisphosphonates. A case report
Fractura bilateral de mandibular tras un tratamiento a largo plazo con bifosfonatos
Actual. Med. 2016; 101: (798): 115-116 DOI: 10.15568/am.2016.798.cc03
Enviado: 23-05-2016
Revisado: 13-06-2016
Aceptado: 18-08-2016
ABSTRACT
Bisphosphonates represent type of medication used for treating numerous pathologies. In fact, more and more clinicians utilize bisphosphonates for dealing oncological diseases, rheumatic pathologies and severe osteoporosis. Despite its benefits, various undesirable side effects have also been associated with the use of these drugs. For instance, patients who receive bisphosphonates present a greater risk of suffering osteonecrosis of jaw. Indeed, the possibility of experiencing this complication is around 0,812% when bisphosphonates are administered intravenously. In contrast, the risk is about 0,01% with oral administration. However, when a tooth extraction is carried out the risk rises to 0,34%. This report presents the case of a 66 years old woman who suffered a bilateral jaw fracture after prolonged treatment with bisphosphonates. Interestingly, no invasive dental procedures were referred by patient. The main aim of this paper is to focus the attention on the serious complications that this treatment may show in the long term.
Keywords: Bilateral jaw fracture, bisphosphonates, jaw bone, ONJ
RESUMEN
Los bifosfonatos son fármacos ampliamente utilizados en el tratamiento de numerosas enfermedades. Diferentes profesionales utilizan los bifosfonatos para tratar complicaciones de patologías oncológicas, osteoporosis y patologías reumatológicas. Sin embargo, a pesar de los efectos benéficos, existen efectos secundarios consecuente al utilizo de este tipo de medicamento. Por ejemplo, la osteonecrosis maxilar es más frecuente en pacientes tratados con bifosfonatos. En este sentido, la posibilidad de desarrollar osteonecrosis maxilar es del 0,812% cuando la medicación es administrada por vía intravenosa y del 0,01% en caso de administración oral. Además, cuando se realiza una extracción dental el riesgo incrementa de un 0,34%. Este artículo presenta el caso de una paciente de 66 años que sufrió una fractura bilateral y espontanea de la mandíbula tras el utilizo de bifosfonatos durante un largo periodo de tiempo. Es importante enfatizar que, en este caso, el paciente no había sido sometido a intervenciones de cirugía oral en los meses previos. El principal objetivo de este estudio es focalizar la atención sobre las posibles complicaciones provocadas por este medicamento.
Palabras clave: Fractura de mandibula bilateral, bifosfonatos, hueso mandibular, osteonecrosis maxilar
Leer Artículo Completo
INTRODUCTION
Several studies demonstrated that Bisphosphonates are an important and well-established drug in the treatment of several diseases (1). Its represent the first-line treatment for malignant hypercalcemia and bone metastasis (2). Moreover, bisphosphonates are also used for treatment of paget’s disease, osteoporosis, and multiple myeloma (3). When administered, bisphosphonates are deposited into the bones, due to high affinity for hydroxyapatite, and are accumulated through time (4). It is common knowledge that patients who receive these medicines have an increased risk of suffering ONJ (5) (6). This risk is around 0,812% if bisphosphonates are administered intravenously. Whereas, is less for oral administration (0,01%). Notwithstanding, the risk rises to 0,34% when invasive dental procedures are performed in patients treated with this drugs (4).In this sense, professionals who prescribe bisphosphonates must strongly advise about this complication and dental extractions should be avoided in these case (7) (8) (9).
CASE REPORTS:
We describe the case of a 66-year-old woman who came to the emergency service of our Hospital with mouth pain, active oral suppuration, fever and bad general condition. Once in the hospital, intravenous antibiotic treatment was administered and a maxillofacial surgeon was contacted. A careful anamnesis revealed that patient received long term therapy with bisphosphonates. In fact, she was diagnosed with breast cancer eight years ago. Intraoral examination showed bone exposure with active suppuration of purulent matter in the third and fourth quadrants of the jaw. The rest of the physical examination was normal. Bearing in mind the patient’s history, we decided to perform an orthopantomography. This test showed a major area of bone degeneration and a bilateral non-displaced fracture of the mandible. Considering all this, the patient was hospitalized in order to maintain intravenous antibiotic treatment. Treatment response was positive since the earliest days. In view of that, we continue with this conservative approach during ten days. We also perform a rigid blockage of the jaw and a complete debridement of necrotic tissue. The clinic substantially improve during the hospital stay. Finally, she was discharged from hospital after two weeks with oral antibiotic for other four weeks. Importantly, jaw blockage was also maintained during 4 weeks. Patient was reviewed every 3-4 weeks for one year. It is important to underline that during the follow-up, we observed that patient remained asymptomatic.
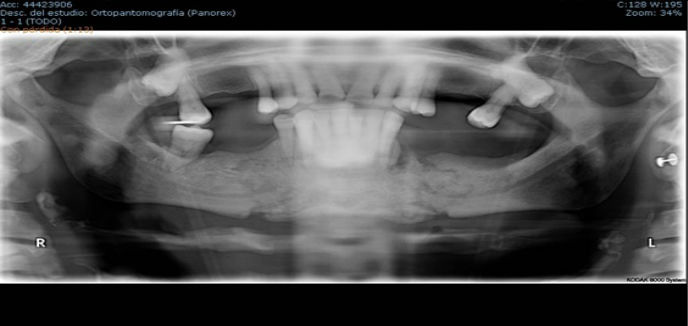
Fig 1. Bilateral jaw fracture.
Fig 2. Jaw fracture evolution during patient follow-up (one months after diagnosis).
Fig 3. Jaw fracture evolution during patient follow-up (nine months after fracture reduction).
DISCUSSION
In recent times, the use of bisphosphonates is growing rapidly. In fact, oral and intravenous preparations of this drugs are daily prescribed for treating pathologies such as osteoporosis, rheumatic pathologies and several metabolic bone diseases. In this light, the main aim of the present report is to show the serious consequences that bisphosphonates could provoke on the jaw bone. In our opinion, these complications are often underestimated by a vast number of clinicians. This report raises three central points. First, conservative treatment is preferable where possible in cases of ONJ. In this line, unnecessary manipulation of the oral cavity should be avoided in these patient. Second, an accurate oral examination is mandatory before the beginning of bisphosphonate treatment. In fact, the existence of dental pathology need to be diagnosed and treated prior to commencement with antiresorptive medication. This attitude might reduce the frequency of ONJ (10). Third, is the consideration that bisphosphonates should be used with caution. In fact, patients who receive bisphosphonates need a close monitoring for life. In addition, there are no effective treatments for this disease.
REFERENCIAS
- R.F. Barghash, W.M Abdou. Pathophysiology of Metastatic Bone Disease and the Role of the Second Generation of Bisphosphonates:From Basic Science to Medicine. Curr Pharm Des. 2016.
- S.L. Ruggiero, T.B. Dodson, L.A. Assael, R. Landesberg, R.E. Marx, B. Mehrotra; American Association of Oral and Maxillofacial Surgeons. American Association of Oral and Maxillofacial Surgeons position paper on bisphosphonate-related osteonecrosis of the jaws. Oral Maxillofac Surg. 2009; 67: 2-12. doi: 10.1016/j.joms.2009.01.009.
- M.J. Rogers, S. Gordon, H.L. Benford, F.P. Coxon, S.P. Luckman, J. Monkkonen, J.C. Frith. Cellular and molecular mechanisms of action of bisphosphonates. Cancer. 2000; 15: 2961-78.
- Advisory Task Force on Bisphosphonate-Related Ostenonecrosis of the Jaws, American Association of Oral and Maxillofacial Surgeons. American Association of Oral and Maxillofacial Surgeons position paper on bisphosphonate-related osteonecrosis of the jaws. J Oral Maxillofac Surg. 2007; 65:369-76.
- F.L Heggendorn, T.C. Leite, K.S. Cunha, A.S. Junior, L.S. Gonçalves, K.B. Da Costa, E.P. Dias. Bisphosphonate-related osteonecrosis of the jaws: Report of a case using conservative protocol. Spec Care Dentist. 2016; 36:43-7. doi: 10.1111/scd.12143.
- F.R. Pires, A. Miranda, E.S. Cardoso, A.S. Cardoso, E.R. Fregnani, C.M. Pereira, M.E. Correa, J.P. lmeida , F. de A Alves , M.A. Lopes, O.P. De Almeida. Oral avascular bone necrosis associated with chemotherapy and biphosphonate therapy. Oral Dis. 2005; 11:365-9.
- C. Walter, M.O. Klein, A. Pabst, B. Al-Nawas, H. Duschner, T. Ziebart. Influence of bisphosphonates on endothelial cells, fibroblasts, and osteogenic cells. Clin Oral Investig. 2010; 14:35-41. doi: 10.1007/s00784-009-0266-4.
- A.A. Polymeri, G.J. Kodovazenitis, A.D. Polymeris, M. Komboli.Bisphosphonates: Clinical Applications and Adverse Events in Dentistry. Oral Health Prev Dent. 2015; 13:289-99. doi: 10.3290/j.ohpd.a34370.
- S. Reiss, D. Sultan. Risk Factors in the Development of Oral Bisphosphonate-induced Osteonecrosis. N Y State Dent J. 2015 Nov; 81:30-3.
- R.H. Goodday. Preventive Strategies for Patients at Risk of Medication-related Osteonecrosis of the Jaw. Oral Maxillofac Surg Clin North Am. 2015; 27: 527-36. doi: 10.1016/j.coms.2015.06.006.
ARTICLE INFORMATION
Corresponding author: Paolo Cariati. Complejo Hospitalario de Granada. Email: paolocariati1@gmail.com