
110
Carlos San Miguel Méndez
Gastroduodenal involvement as an unusual presentation of Crohn’s disease
RESULTS:
The immediate post-operative course in the first case was
uneventful and several months following discharge the patient
continues with proper oral tolerance. Imaging studies upon
ultrasound revealed no further passage impairment neither
gastroduodenal nor ileal.
The Pathology report was described as fragments of
moderate chronic non-specific inflammation, mild epithelial
dysplasia and ulceration foci.
The post-operative period was also uneventful in our second
case, and on the third day the patient started to drink liquids. She
was discharged one week later with no surgical complications.
During her follow-up consultations, there have been no symptoms
or findings suggestive of relapse. Indeed, she has proper oral
tolerance, having gained 6 kg weight.
Her mild affection at the colon frame is still objective upon
colonoscopy but without any clinical manifestation.
DISCUSSION:
CD can involve any part of the gastrointestinal tract; however,
there are few reports on the pathology and treatment of gastric
lesions in this disease, which led the interest of our case report.
Gastroduodenal involvement of CD is present in 30% of
cases but being symptomatic in only 0.5% to 4% of them (1), and
almost all have simultaneous affectation of the terminal ileum or
large intestine, as in our cases (2, 3, 4, 5).
The most common symptom, epigastric postprandial pain, is
usually relieved by food intake or antiacids. Continuous abdominal
pain, associated with nausea and vomiting, weight loss, and
anorexia, suggests difficulties in gastric emptying probably due to
gastroduodenal stenosis (3). However, these symptoms may also
be attributable to ulcer disease or treatment side effects, making
the clinical suspicion and the ruling out very important. In this
context, it should be underlined that the prevalence of
H. pylori
infection in these patients is similar to the general population
(2,3).
Histological findings may often be non-specific in CD
(1, 5), as in our two patients. Nevertheless, despite a clear
history of inflamatory bowel disease, an UE biopsy is always
recommended.
Traditional imaging in CD has included ultrasound and
CT. At present, magnetic resonance enterography provides
excellent soft tissue contrast resolution, potential for dynamic
assessment of the bowel, and lack of ionizing radiation (5), thus
offering considerable information about disease extent, activity,
and complications. The sensitivity of MRI to diagnose fistulae
(94.9%), abscesses (93.8%), and strictures (96.2%) supports its
use as a superior imaging modality for complication assessment
in CD.
Unfortunately, pyloric stenosis does not allow an
adequate bowel preparation, and thus could not be of interest
in gastroduodenal stenosis of CD. In patients with CD, mucosal
disease activity is routinely assessed by endoscopy and histologic
evaluation, but in recent studies it has been evaluated the
translational potential of noninvasive 18F-FDG PET/CT for the
assessment of mucosal damage in CD, as we have done in our
second case report (6). The usefulness of this method becomes
relevant as an alternative to MRI enterography in the group of
patients in which it is not possible to perform an adequate bowel
preparation, as in our second case.
Approximately one third of all patients does not respond to
medical treatment and requires surgery. Obstruction and gastric
emptying difficulty are the most common indications (5).
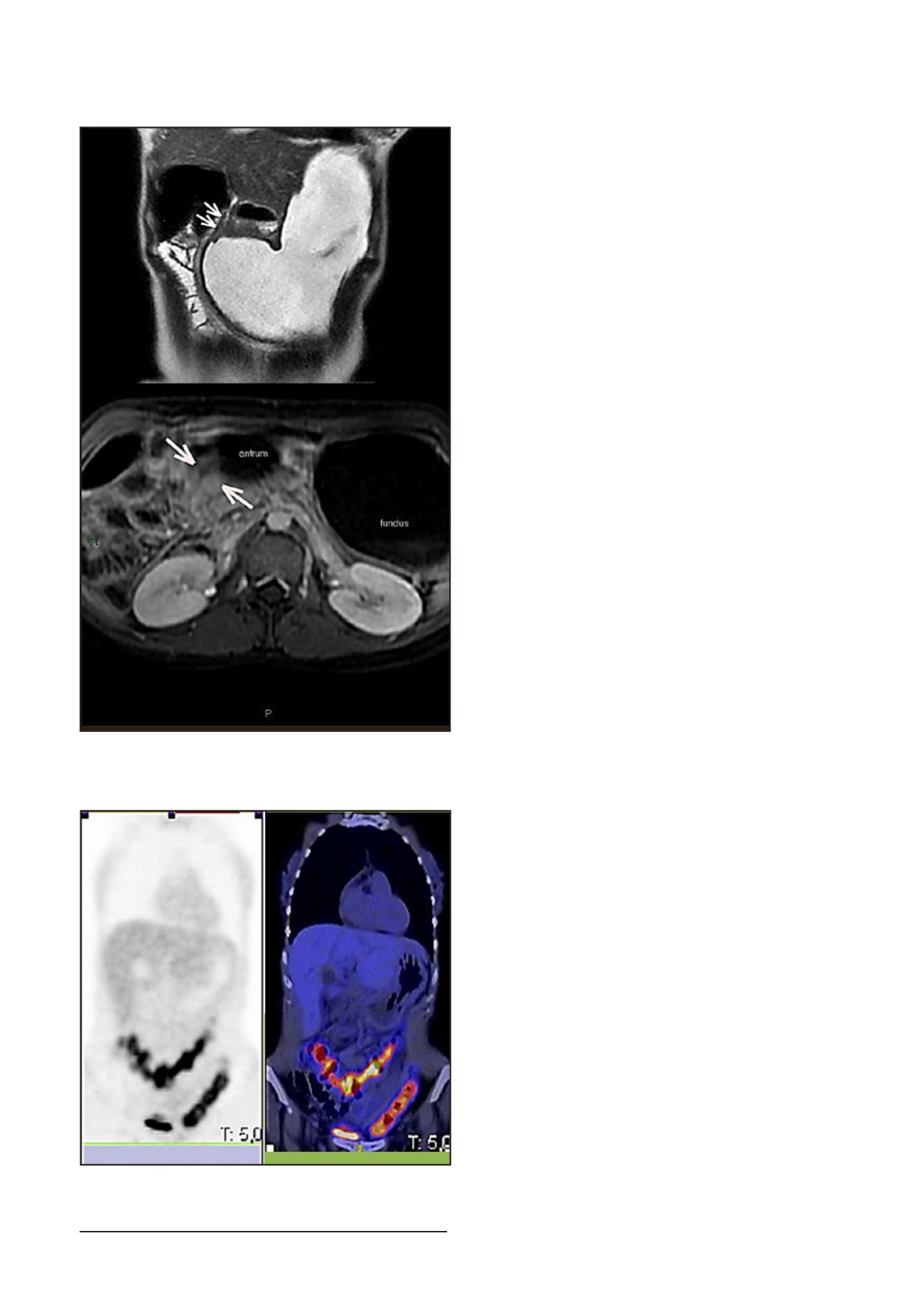
Fig1. A.MRI Enterography. Important gastric distensionand reductionof
the lumenof the pyloric regionandfirst duodenal portion. B. AxialMRI
Enterography: Pyloric stenosiswithunstratifiedhomogeneous uptake.
Fig 2. 18FDG-PET/CT: Increase of metabolism at the colic framework.

















